UofL Health reports 23 frostbite patients as doctors outline prevention, warning signs and first-aid steps
A spike in cold-injury cases
UofL Health has treated 23 patients for frostbite, underscoring how quickly cold exposure can turn into a medical emergency during periods of low temperatures and strong wind. Frostbite occurs when skin and the tissue beneath it begin to freeze, most often affecting fingers, toes, ears, and the nose. Clinicians note that the condition can be difficult to recognize early because numbness may prevent people from realizing an injury is developing.
How frostbite develops and what it looks like
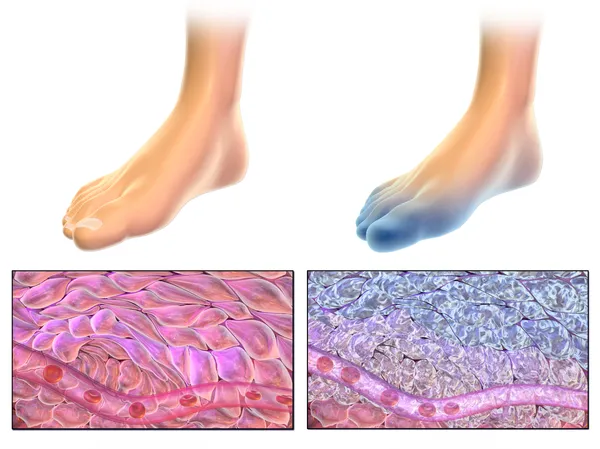
Frostbite typically starts with cold skin and a prickling sensation. As exposure continues, symptoms can progress to numbness, skin color changes (including red, white, bluish-white, or grayish-yellow), and skin that appears hard or waxy. More severe injuries can blister after rewarming and may involve deeper tissue damage.
In extreme wind chill, frostbite can occur on exposed skin in less than 30 minutes.
Prevention: the practical steps that matter most
Doctors emphasize that most frostbite cases are preventable when people anticipate conditions and limit exposure. Protective choices become more important in wet or windy weather and when clothing restricts circulation.
- Limit time outdoors in cold, wet, or windy conditions and factor in wind chill when planning activities.
- Dress in multiple loose layers; use windproof and waterproof outerwear to block wind and moisture.
- Change out of wet clothing promptly, particularly gloves, hats, and socks.
- Cover high-risk areas: ears with a hat or headband, and hands with mittens (often warmer than gloves).
- Wear well-fitting socks and insulated boots; avoid footwear that is too tight and can reduce blood flow.
- Avoid alcohol, which can increase heat loss and impair judgment about cold exposure.
What to do if you suspect frostbite
Clinicians advise getting out of the cold immediately and seeking shelter. Early recognition is key: if skin becomes pale, waxy, or numb, treat it as a warning sign rather than waiting for pain. Medical evaluation is recommended because frostbite can damage skin, muscle, and even bone, and severe cases can lead to infection or nerve injury.
For suspected frostbite or worsening symptoms, patients are urged to seek medical attention promptly—especially if pain increases, swelling develops, or skin changes persist after attempts to warm up.
Why the 23 cases matter for Louisville
The number of patients treated highlights the broader strain that harsh winter conditions can place on emergency care. Frostbite often accompanies other cold-weather risks, including hypothermia and falls, making preparation and early action central to reducing avoidable injuries during cold snaps.